Breast cancer is the most frequently occurring cancer in women of reproductive age. With advancements in early diagnosis and treatment options, more women diagnosed with breast cancer are living longer today than ever before. However, systemic treatments may adversely affect childbearing plans.
During this time, patients are often overwhelmed with news of their diagnosis and possible treatment plans and it is important for providers involved in their care to ask whether fertility preservation is desired. Fortunately, the use of assisted reproductive technologies and therapies for ovarian protection improve fertility prospects for most patients. Often times, there is minimal to no treatment delay as egg or embryo banking can be performed prior to necessary cancer treatments.
Individuals with BRCA+ or other similar genetic testing leading to increased risk for breast cancer may consider genetic testing of embryos (PGT-A) to prevent the passage of genetic mutations to their future children.
The HART Fertility Clinic physicians are committed to providing patients with immediate assistance in coordinating care that aims to achieve each individual patient's reproductive goals. They work hand in hand with organizations such as Livestrong and local grant organizations to provide discounts and help relieve the financial burdens often associated with a new cancer diagnosis.
We urge women and men alike to talk with their health care providers and ensure breast cancer screening be performed if advised. Risk factors for breast cancer may include but are not limited to age, female sex, obesity, family history of breast, ovarian or uterine cancer, certain genetic predispositions, and reproductive history.
By:

Dr. Toral Parikh, MD

IUI, which stands for Intrauterine Insemination, is one of the simpler procedures we offer at Hart Fertility Clinic in Kingwood and The Woodlands. It is ideal for women who are experiencing unexplained infertility and/or their partner experiences sperm abnormalities. IUI is meant as a boost and serves to increase how much sperm can travel, resulting in an improved chance of fertilization.
How Does An IUI Procedure Work?
Evaluation Prior to Infertility Treatment
First of all, if you are worried about how long it has taken you to get pregnant, you should first speak with a doctor and voice your concerns. Your doctor will ask you questions relating to yours and your partner's individual medical histories and sexual histories. After this, your doctor will administer specialized tests, such as a semen analysis and a fallopian tube evaluation to determine if infertility is something you and your partner should be concerned with and what your options are.
IUI is often the first form of treatment, especially if your infertility seems unexplained or if your partner's sperm motility is an obstacle.
Prior to Intrauterine Insemination
Once your doctor has determined that IUI is a viable treatment option for you, you may be given ovulation-stimulating medication. Our North Houston fertility specialists will closely monitor you as you take these medications so we know when your eggs are mature. Within 24-36 hours of your eggs maturing, we will perform the procedure.
If you suffer from endometriosis, you may also be given medications that encourage good quality eggs, in addition to the ovulation-stimulating medications. This will ensure you have a good egg for the procedure.
Performing an IUI Procedure
Your partner, or a donor if that is what you and your partner wish, will provide us with a semen sample, which will be taken to a lab and specially washed to separate the semen from its fluid. This also helps separate the lower quality sperm from the more motile sperm. We will then insert the semen directly into the uterus to ensure as many sperm cells as possible are placed in the uterus, which offers a boost and increases your possibility of conceiving. The process only takes a few minutes and is absolutely pain-free.
IUI Infertility Treatment at Our North Houston Fertility Clinic
Infertility is a challenge, but our team at Hart Fertility is here to support you the entire way and offer you the best care possible. If you and your partner are candidates for Intrauterine Insemination and would like to discuss it in more detail, please book an appointment with us.

Infertility is far more common than you may think. It's a deeply personal challenge and can weigh you down, but there are ways to improve your chances of delivering a healthy baby. When in conjunction with infertility treatment, a fertility-boosting diet may also help you achieve a healthy birth. Here are some of the practices our Houston fertility specialists recommend.
Eat Foods Rich in Antioxidants
Antioxidants attack free radicals that enter your body. In essence, free radicals are unbalanced atoms that can severely damage your cells which cause harm and aging. This means they can easily damage both sperm cells and egg cells. Antioxidant-rich foods include Vitamin C and E, folate, and beta carotene. You can find these in many fruits, nuts, and veggies.
Avoid Trans Fats
There are some healthy fats, like omega-3 fatty acids that are found in salmon and avocado, that can boost fertility. But there are also bad fats known as trans fats, which may hinder fertility. They are easily found in fried foods, processed snacks, and margarine. Trans fats have been associated with infertility because they have bad effects on insulin sensitivity.
Try A Low-Carb Diet
If you are one of many who experience infertility as a result of Polycystic Ovary Syndrome (PCOS), a low carb diet is recommended because it helps maintain healthy weight, reduce insulin, and helps regulate your menstrual cycle. It has also been shown that eating a low-carb diet helped reduce testosterone and insulin levels, which, if too high, can lead to infertility.
Decrease How Many Refined Carbs You Eat
It's clear that the amount of carbs you eat is important when trying to achieve a healthy birth, but the kind of carbs you eat matter too, especially if you suffer from PCOS. Refined carbs, in particular, should be avoided. These can be consumed in sugary foods and drinks and processed grains, such as pasta and bread. The reason we recommend avoiding refined carbs when struggling with PCOS and fertility is because they can very quickly raise your blood sugar levels.
Replacing Animal Protein
Animal proteins, such as red meat, fish, and eggs can be replaced by vegetable proteins. Vegetable proteins are those that come from beans, legumes, nuts, and seeds. These have been shown to help offer a fertility boost, but they are also good for your overall health because they are rich in vitamins and minerals.
Our Houston Fertility Clinic Recommends You Take Good Care of Your Wellbeing
When going through infertility treatment, it is especially important to be at your best health to increase your chances. Contact our Houston fertility clinic today so we can help you establish a healthy lifestyle through the course of your treatment.

IVF stands for In Vitro Fertilization and is a popular method used for couples to become pregnant. Here are some important facts to know if you are considering this fertility treatment in The Woodlands and Kingwood areas of Houston.
1. IVF Shouldn't be Your First Course of Action if You're Having a Hard Time Getting Pregnant
Getting pregnant can take some longer than others and it does not necessarily mean a woman is infertile. If you are feeling concerned because you think it's taking too long, speak to your doctor about it before anything else. When you speak with your doctor, he or she will first ask about your medical and sexual history, as well as that of your partner's. Next, tests such as semen analysis, fallopian tube evaluation, and ovarian reserve tests will be administered. Gathering this information helps your doctor determine if infertility is indeed the case and what exactly is causing it. Afterward, your doctor will walk you through all of your options and let you know if IVF treatment is recommended.
2. The Younger You Are, The Better Your Chances of Becoming Pregnant
Even healthy young women can have a hard time conceiving and may be candidates for In Vitro Fertilization. At a mere 30 years of age, it's normal to have some eggs that are out of the ordinary that cannot become properly fertilized. Women younger than 35 typically have better chances of conceiving and delivering a healthy baby, but that doesn't mean its impossible for women above that age. There have, in fact, been some success cases for women above 35 at our North Houston fertility clinic.
3. Your Lifestyle Can Affect The Outcome of IVF Treatment
It's no secret that a healthy lifestyle equals a healthy, medically-sound body. BMI and how often both partners in the relationship exercise can have an effect on whether they achieve a successful birth. At our Houston fertility clinic in The Woodlands and Kingwood, we recommend a diet rich in protein and vegetables to help improve and encourage embryo quality. Having an unhealthy lifestyle and habits can harm your chances of achieving a successful pregnancy, so we also recommend getting enough sleep (7-9 hours a night) and avoiding the consumption of alcoholic drinks, as these practices can lead to a lower rate of pregnancy.
Schedule Your First Visit With HART Fertility Clinic in North Houston
If IVF treatment has been recommended to you, please request an appointment so we can take the first step toward developing a relationship with you. Don't hesitate to ask any questions prior to your first visit so that we can ensure you have a pleasant experience.
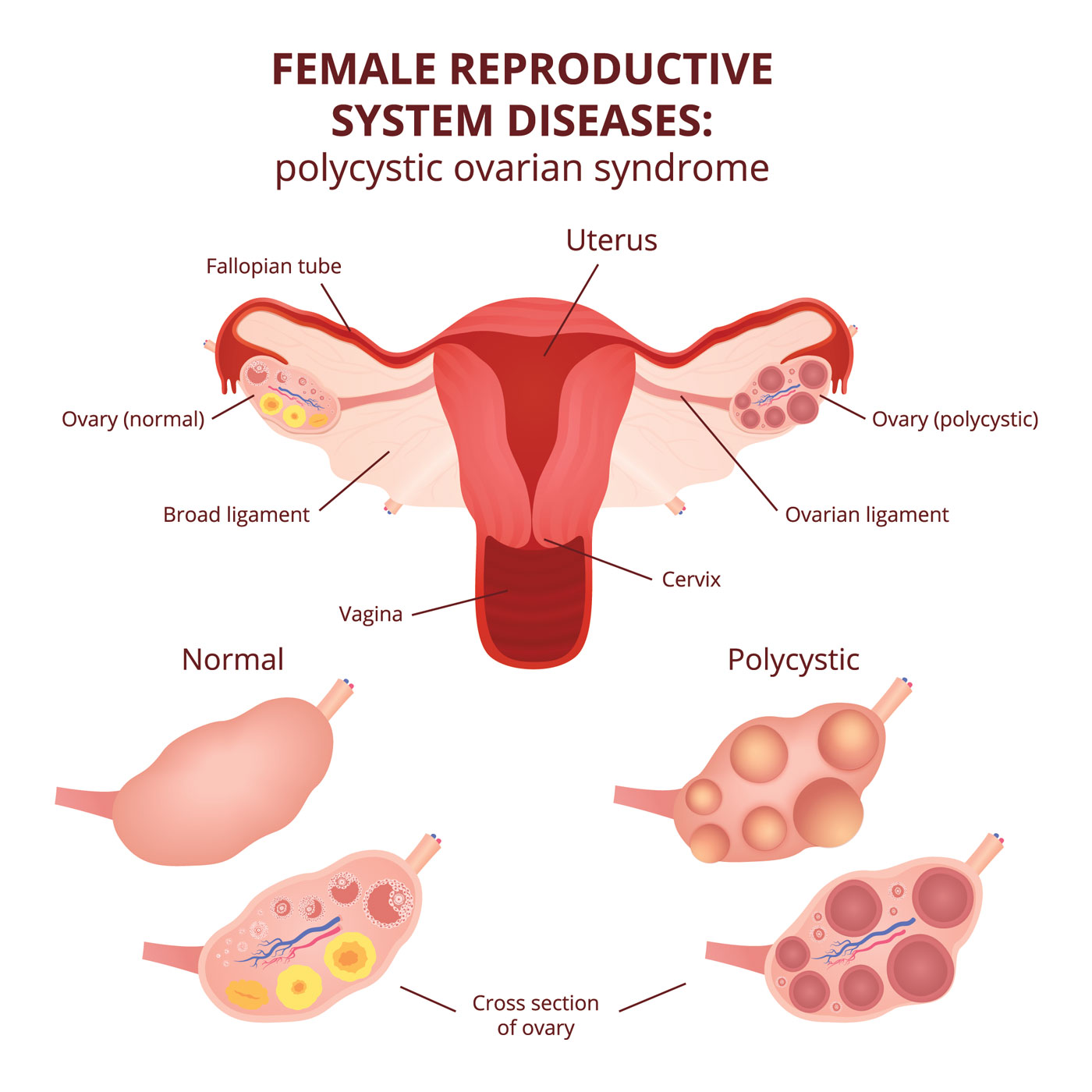
September is Polycystic Ovary Syndrome (PCOS) awareness month. PCOS is the most common reproductive endocrine disorder. It is a life-long disorder which presents with different symptoms at various stages of life. Symptoms include irregular periods due to lack of ovulation, excessive hair growth and acne in adolescence and early adulthood. Weight gain can frequently accompany PCOS which may lead to medical issues seen later in life such as metabolic syndrome. Metabolic syndrome is a constellation of symptoms including insulin resistance leading to prediabetes or overt diabetes, high cholesterol, and high blood pressure. Women with prolonged amenorrhea also may be at risk for uterine cancer later in life.
The diagnosis of PCOS is simple and can be mostly achieved based on clinical presentation. Irregular menses, such as going months without a period due to lack of ovulation, excessive hair growth and/or acne/oily skin may be sufficient to make the diagnosis. An ultrasound exam may be helpful establishing the diagnosis but not always necessary if women have the aforementioned symptoms. Blood work may be necessary if your physician is concerned about other disorders that may present like PCOS.
The treatment depends on the patient’s age and the goals she would like to achieve. If the goal is to get pregnant, the majority of women respond simple oral fertility treatments such as clomiphene or letrozole. In some women, further treatments may be necessary such as injectable hormone therapies to induce ovulation or in vitro fertilization (IVF). If reproduction is not an immediate goal then control of menstrual cycles and metabolic syndrome is of utmost importance. Menstrual cycles can be regulated using birth control pills or cyclic progesterone pills. Metabolic syndrome can be best controlled through weight loss. Combination of diet and exercise is required to prevent weight gain or to achieve weight loss. Studies have shown that 10% weight loss may resume ovulation in up to 90% of women. High protein and low carbohydrate diets have been shown to successfully assist in desired weight loss.
Your physician at HART Fertility can help assist proper diagnosis and management of PCOS. For help, call us and schedule an appointment to discuss your health and reproductive goals today.